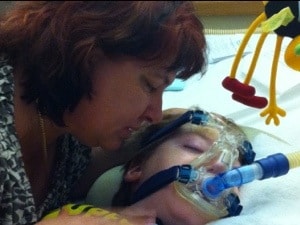
Samuel remains in hospital and the watching and waiting for the spark in his eyes to burst into flame continues.
In a recent status update on Facebook I described the experience being like taking one step forward, three sideways and one back… while adding in a triple somersault in a half pike position.
If that sounds like it is a degree of difficulty of around 9.0 then the thoughts and discussions that we are having have a degree of difficulty of 10.0…..Thinking about issues of death and dying are nothing new on this blog, or indeed new to Samuel’s circumstances. However, with every new twist decisions become more palpable and pressing.
What is happening with Samuel?
It was all looking good, or should I say better. Increased alertness, noise making.. better air entry in both lungs, saturation levels looking ok, blood gas levels ok, and then…..
The temperature spiked, his work of breathing increased.. he went from his nasal Bi-Pap mask back to his full face Bi-Pap mask and his pressures needed to be increased again.. extreme difficulty drawing blood for the necessary tests, blood coagulating very quickly, blood gases being a bit out of whack and continuing problems with his electrolyte levels.. particularly being a bit low on potassium (important for regulating things like the heart rhythm).. and he has less of the life and spark in his eyes again.
Then some results come back and one of the bugs in his lungs has mutated and is becoming increasingly resistant to the antibiotics (which are already in the “last line of defence” category).
What does it all mean?
If only there was a simple answer to that question. What it means is more questions than answers.
I’ve always been interested in the question about what constitutes a good life, but know its time to also contemplate the question about what constitutes a good death?
Where do you look for advice like that?
Our experience with all of Samuel’s doctors and nurses at the Childrens Hospital at Westmead (CHW) has been an overwhelmingly positive one, and they are all doing what they can to sit with us and discuss questions about what is happening to Samuel, what it means and the type of decisions we may have to make.
The World Health Organisation defines palliative care as “the active and total care of the child’s body, mind and spirit, and also involves giving support to the child’s family”. Our teams at CWH really are doing a great job of meeting this definition.. as they have across the years. The conversations are just becoming more intense, more focused and in some ways more specific around treatment decisions.
There are some decisions that we may be forced to make, and there are some that Samuel or circumstances will dictate and/or take out of our hands.
What is a good and natural death?
We already have, and have had for quite a while an “Allow Natural Death” order in place, limiting the scope of treatment that can be implemented in the case that Samuel goes into respiratory or cardiac arrest.
I have read a fair bit around the associated decision making, including reading the “Decision Making at the end of life in infants, children and adolescents” Policy document of the Royal Australasian College of Physicians, so that I can really understand where some of the obligations, rights and responsibilities of our medical teams are coming from.
It sets out principles including Respect for Life, A duty to act in the best interests of the child, and palliative care, Autonomy and Competence and Right to information and choice. It includes discussion about withholding or withdrawing treatment, It even includes a section dealing with Severe Neuorlogical Impairment.. clearly where Samuel fits.
It talks about quality of life….. and how subjective that issue is.. as conditions progress what really is quality of life??
I’ve also read a few other bioehtics articles around end of life decision making.. some of these involve discussion of concepts like “a life worth living” and “a life not worth living” and “determining thresholds”. as harsh as they sound from a “medical professional” point of view all of the concepts used make sense.
BUT WHAT ABOUT….
It doesn’t matter how much sense all the policy documents and academic bioethics papers make.. what about when it is your child??
Being confronted with the REAL questions about what is the plan from here, what will we consider, what wont we consider, when will we make decisions about different aspects of treatment none of those arguments matter.. it is simply gut wrenching and there are no answers.
I referred to courage again in the last couple of posts… but I don’t know what courage looks like here. Yes I’ll whisper to myself that I’ll try again tomorrow, yes tomorrow we will be thinking about these things again.. the answers probably won’t be any clearer.
Right now the issue is about overcoming my own fear about making the right decisions for Samuel. Decisions that will keep him as comfortable as possible, not allow him to be overly distressed and ultimately to try and make sure that he does not die on his own when that time comes (even though that is something we simply can’t control.)
Then again…
Samuel always has his way, and he is just as likely to turn around, pick up and look at as like “whats all the fuss, let’s go home” (and do this all again some other time!)